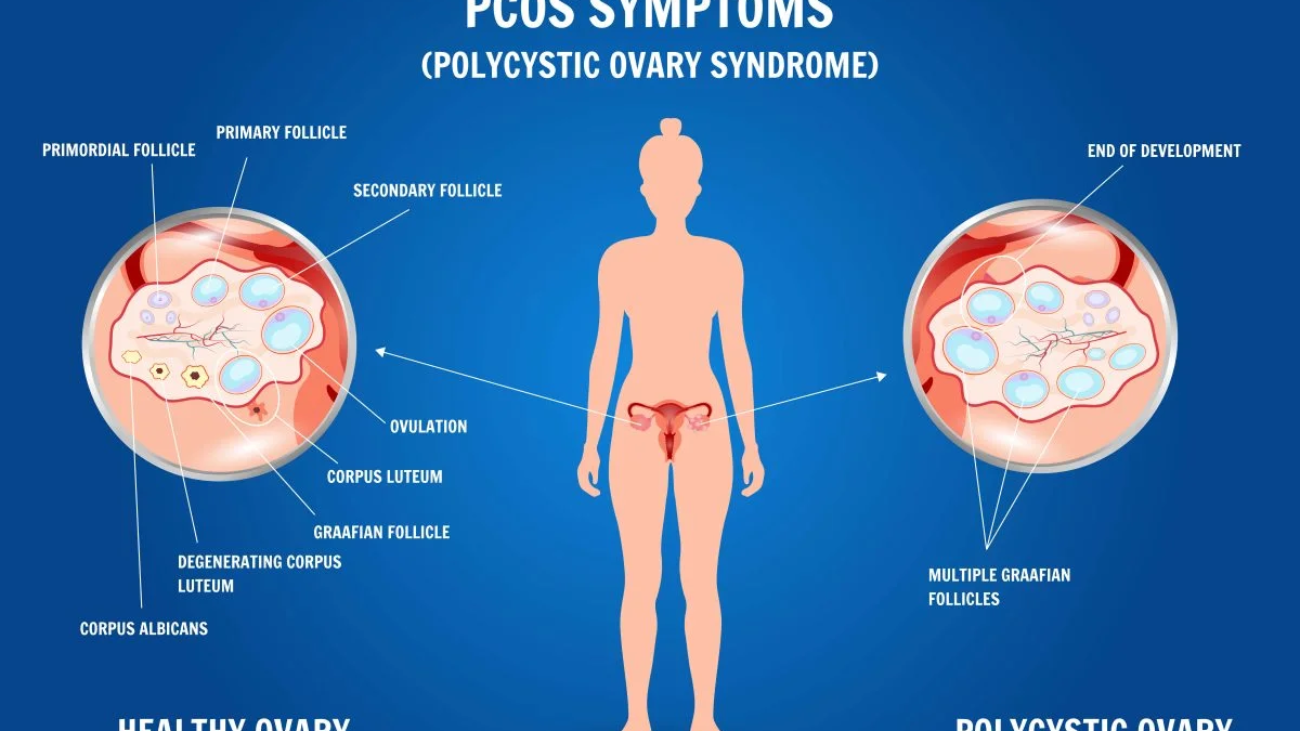
Menstrual Hygiene: Your Guide to Sustainable, Zero Waste Periods
Menstrual hygiene is a crucial aspect of women’s health, yet it is often overlooked or surrounded by stigma. In many parts of India and the world, open conversations about menstruation are still emerging. As awareness increases, more women are exploring sustainable and zero-waste period products that are healthier for the body and the environment.
Sustainable menstrual hygiene practices not only support better reproductive health, but also reduce environmental waste and promote confidence and dignity during menstruation.
Understanding the importance of menstrual hygiene and choosing the right products can help women manage their periods safely and comfortably.
If you want expert guidance on menstrual health or menstrual concerns, consulting an experienced gynecologist like Dr. Nitasha Gupta can help you make informed decisions about your reproductive health.
Learn more:
https://www.drnitashagupta.com/about/
What Is Menstrual Health and Hygiene?
Menstrual health refers to a woman’s overall physical, emotional, and social well-being during menstruation.
Menstrual hygiene involves the daily practices that help maintain cleanliness and prevent infections during a period. These include:
- Regularly changing menstrual products
- Washing the genital area with clean water
- Practicing proper hand hygiene
- Safely disposing of or cleaning menstrual products
However, menstrual hygiene goes beyond cleanliness. It also includes comfort, access to safe menstrual products, education about menstrual health, and the ability to manage periods with dignity.
Good menstrual hygiene practices are essential for preventing infections and maintaining reproductive health.
Why Menstrual Hygiene Is Important
Maintaining proper menstrual hygiene is vital for both physical and mental well-being.
Prevents infections
Proper hygiene helps reduce the risk of:
- urinary tract infections (UTIs)
- reproductive tract infections
- skin irritation and rashes
Supports emotional well-being
When women have access to safe menstrual care, they experience:
- greater confidence
- reduced anxiety
- improved participation in daily activities
Protects reproductive health
Good menstrual hygiene reduces the risk of long-term reproductive health complications.
Encourages menstrual awareness
Understanding menstrual hygiene empowers women to make informed decisions about their bodies and health.
Physical and Mental Effects of Poor Menstrual Hygiene
Neglecting menstrual hygiene can have serious health consequences.
Physical health risks
Poor hygiene during menstruation may lead to:
Skin irritation and rashes
Using damp or unclean materials for long periods may cause irritation or infection.
Urinary tract infections (UTIs)
UTIs may cause symptoms such as:
- burning during urination
- pelvic discomfort
- frequent urge to urinate
Reproductive tract infections
Infections can spread to the uterus and fallopian tubes, sometimes leading to pelvic inflammatory disease (PID).
Toxic shock syndrome (TSS)
A rare but serious condition caused by bacterial toxins when tampons or menstrual cups are left in for too long.
Increased risk of reproductive health complications
Repeated infections may lead to long-term complications if untreated.
Psychological and social effects
Poor menstrual hygiene can also affect mental health.
Women and girls may experience:
- embarrassment or stigma
- anxiety and social withdrawal
- missed school or work days
- reduced self-confidence
These challenges highlight the importance of improving menstrual awareness and access to hygiene products.
Types of Menstrual Hygiene Products
Today, women can choose from a variety of menstrual products depending on comfort, lifestyle, and sustainability preferences.
Disposable sanitary pads
Sanitary pads are absorbent products worn in underwear to collect menstrual blood.
Key points:
- widely available and easy to use
- should be changed every 4–6 hours
- contribute significantly to menstrual waste
Tampons
Tampons are inserted into the vagina to absorb menstrual blood.
Important guidelines:
- available in different absorbency levels
- should be changed every 4–6 hours
- prolonged use may increase the risk of toxic shock syndrome
Reusable cloth pads
Reusable cloth pads are washable alternatives to disposable pads.
Benefits include:
- environmentally friendly
- reusable for up to 2–4 years
- cost-effective over time
However, they require proper washing and drying to maintain hygiene.
Menstrual cups
Menstrual cups are flexible silicone cups inserted into the vagina to collect menstrual blood.
Advantages:
- reusable for 5–10 years
- can hold more blood than pads or tampons
- need to be emptied every 6–12 hours
Menstrual cups are becoming increasingly popular due to their minimal environmental impact.
Period panties
Period underwear contains absorbent layers that collect menstrual blood.
Features include:
- comfortable and reusable
- suitable for light to moderate flow
- washable and eco-friendly
What Is Menstrual Hygiene Management?
Menstrual hygiene management (MHM) refers to a comprehensive approach that ensures menstruation is managed safely and with dignity.
It includes three key components:
- Education about menstrual health and hygiene
- Access to safe menstrual products
- Clean and private facilities for changing and disposal
Effective menstrual hygiene management improves both health outcomes and quality of life.
Causes of Poor Menstrual Hygiene
Several factors contribute to poor menstrual hygiene practices.
Common causes include:
- limited access to affordable menstrual products
- lack of sanitation facilities
- insufficient menstrual education
- social stigma and cultural taboos
- financial constraints
Addressing these challenges requires education, community awareness, and improved access to menstrual care resources.
Benefits of Sustainable Period Practices
Sustainable menstrual hygiene focuses on reducing waste and promoting reusable products.
Reduced environmental impact
Disposable pads and tampons often contain plastic that can take hundreds of years to decompose.
Cost savings
Reusable products like menstrual cups or cloth pads last for years, reducing long-term costs.
Reduced chemical exposure
Eco-friendly products often avoid synthetic materials and harsh chemicals.
Greater menstrual awareness
Sustainable menstrual practices encourage women to better understand their menstrual cycles and health.
Tips for Adopting Sustainable Period Practices
Transitioning to sustainable menstrual care can be gradual and personalized.
Here are some helpful tips:
- Start with one reusable product such as a cloth pad or menstrual cup
- Maintain proper hygiene by washing reusable products regularly
- Use mild soap and clean water when cleaning menstrual products
- Dry reusable products in sunlight for natural disinfection
- Carry reusable products in clean, breathable pouches
- Track your menstrual cycle to stay prepared
- Dispose of non-reusable waste responsibly
Sustainability does not require immediate changes. Choose options that match your comfort and lifestyle.
Sustainable Menstrual Products
Several products support zero-waste menstrual practices.
Menstrual cups
Reusable silicone cups that can last up to 10 years with proper care.
Cloth pads
Washable pads that last 2–4 years and reduce disposable waste.
Period underwear
Reusable absorbent underwear suitable for lighter flow days.
These alternatives support both environmental sustainability and menstrual comfort.
When Should You Consult a Gynecologist?
While menstrual hygiene products help manage periods, certain symptoms require medical advice.
Consult a doctor if you experience:
- severe menstrual pain
- extremely heavy bleeding
- irregular or missed periods
- unusual vaginal discharge
- persistent discomfort during menstruation
An experienced gynecologist like Dr. Nitasha Gupta can provide expert guidance on menstrual health and reproductive care.
Book an appointment:
https://www.drnitashagupta.com/contact/
Conclusion
Menstrual hygiene is essential for protecting both women’s health and environmental sustainability. By practicing proper hygiene, choosing safe menstrual products, and adopting sustainable period solutions, women can manage menstruation with comfort, confidence, and dignity.
Sustainable menstrual practices not only reduce environmental waste but also promote greater awareness of reproductive health.
With education, access to resources, and supportive healthcare, menstrual care can become a healthier and more empowering experience for women everywhere.
Frequently Asked Questions (FAQs)
What is menstrual hygiene?
Menstrual hygiene refers to the practices that help maintain cleanliness and prevent infections during menstruation.
How often should menstrual products be changed?
Pads and tampons should generally be changed every 4–6 hours to maintain hygiene and prevent infections.
Are menstrual cups safe?
Yes. When used and cleaned properly, menstrual cups are safe and can last up to 10 years.
What are zero-waste period products?
Zero-waste menstrual products include reusable options like menstrual cups, cloth pads, and period underwear that reduce environmental waste.
Why is sustainable menstrual hygiene important?
Sustainable menstrual hygiene reduces environmental impact, lowers long-term costs, and supports healthier menstrual care practices.
Internal Links
Women’s health consultation
https://www.drnitashagupta.com/
About Dr Nitasha Gupta
https://www.drnitashagupta.com/about/
Book appointment
https://www.drnitashagupta.com/contact/
External Resource
Cosmetic Gynecology & Intimate Wellness
https://labellacosgyn.com/