Low Sperm Count in Men: Symptoms, Causes & When to Worry
Male fertility problems are becoming increasingly common today. One of the most common causes is low sperm count, also known as male factor infertility.
Many men experience fertility issues silently because symptoms often go unnoticed until pregnancy planning begins.
Understanding the early signs, causes, and treatment options can help improve fertility outcomes and reproductive health.
If you are searching for:
- low sperm count symptoms
- male infertility causes
- fertility problems in men
- low sperm motility
- difficulty conceiving
- male fertility specialist near me
this guide explains everything men should know about low sperm count and reproductive health.
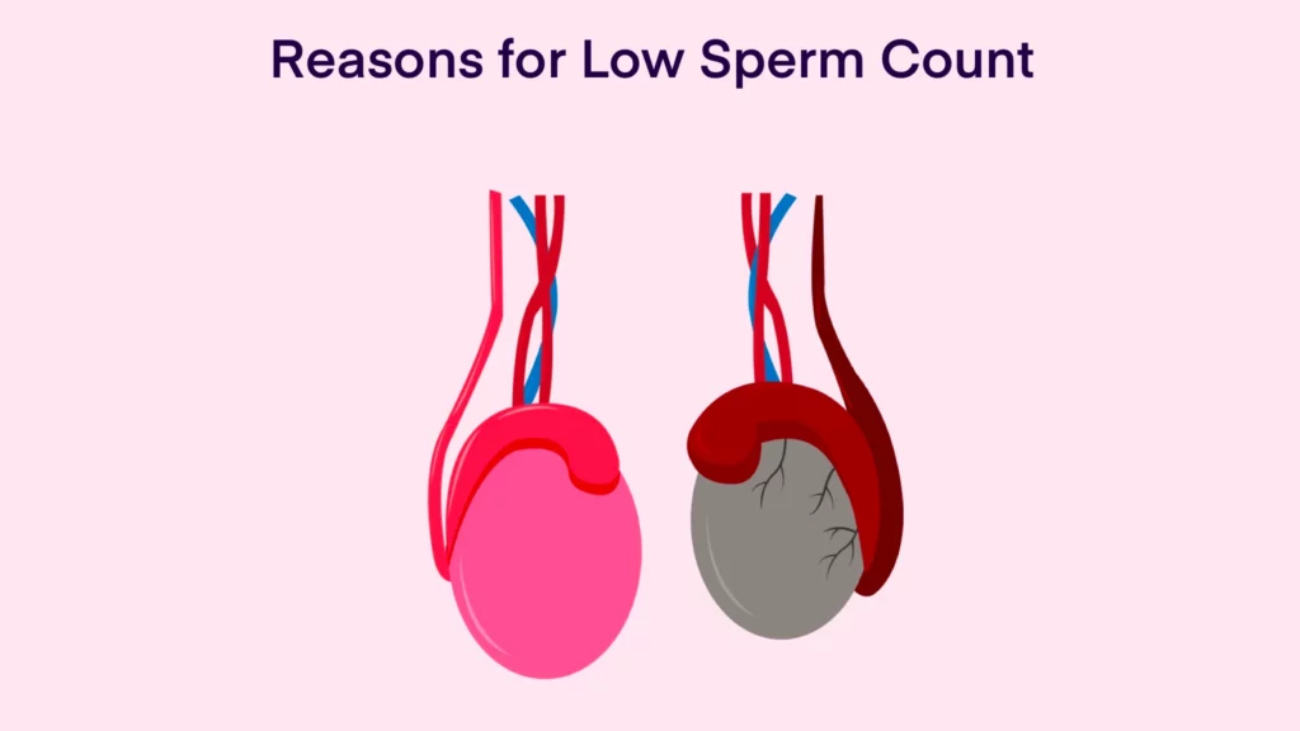
What Is Low Sperm Count?
Low sperm count means the semen contains fewer sperm than normal during ejaculation.
A lower sperm count can reduce the chances of fertilizing an egg naturally.
According to World Health Organization (WHO), sperm concentration below normal reference levels may affect fertility potential.
Sperm health depends on:
- sperm count
- sperm motility
- sperm morphology
- semen quality
Common Symptoms of Low Sperm Count
In many cases, low sperm count causes no obvious symptoms.
However, some men may experience:
- Difficulty conceiving
- Reduced sexual desire
- Erectile dysfunction
- Pain or swelling in testicles
- Hormonal imbalance signs
- Decreased facial or body hair
Most men discover fertility issues only after trying for pregnancy for several months.
Early Signs Men Often Ignore
Low Energy Levels
Hormonal imbalance can sometimes affect energy and stamina.
Reduced Libido
Low testosterone may impact sexual drive.
Difficulty Achieving Pregnancy
One of the biggest warning signs is difficulty conceiving despite regular unprotected intercourse.
Testicular Discomfort
Pain, heaviness, or swelling may require medical evaluation.
Common Causes of Low Sperm Count
Lifestyle Factors
Modern lifestyle habits can strongly affect male fertility.
Common risk factors include:
- smoking
- alcohol consumption
- obesity
- stress
- poor sleep
- unhealthy diet
- lack of exercise
Excessive Heat Exposure
Frequent exposure to heat may affect sperm production.
Examples include:
- hot tubs
- saunas
- prolonged laptop use
- tight underwear
Hormonal Imbalance
Hormones play a major role in sperm production and reproductive health.
Medical Conditions
Certain medical conditions may affect fertility:
- diabetes
- infections
- varicocele
- hormonal disorders
- sexually transmitted infections
Poor Sperm Motility
Even if sperm count is normal, poor sperm movement can reduce fertility chances.
Can Low Sperm Count Cause Infertility?
Yes.
Low sperm count is one of the leading causes of male infertility worldwide.
Men searching for:
- why pregnancy is not happening
- fertility problems in men
- male infertility treatment
often discover sperm quality issues during fertility testing.
According to Indian Council of Medical Research (ICMR), male factors contribute significantly to infertility cases in couples.
How Is Low Sperm Count Diagnosed?
Diagnosis usually includes:
Semen Analysis
Checks:
- sperm count
- motility
- morphology
- semen quality
Hormonal Testing
Evaluates testosterone and reproductive hormones.
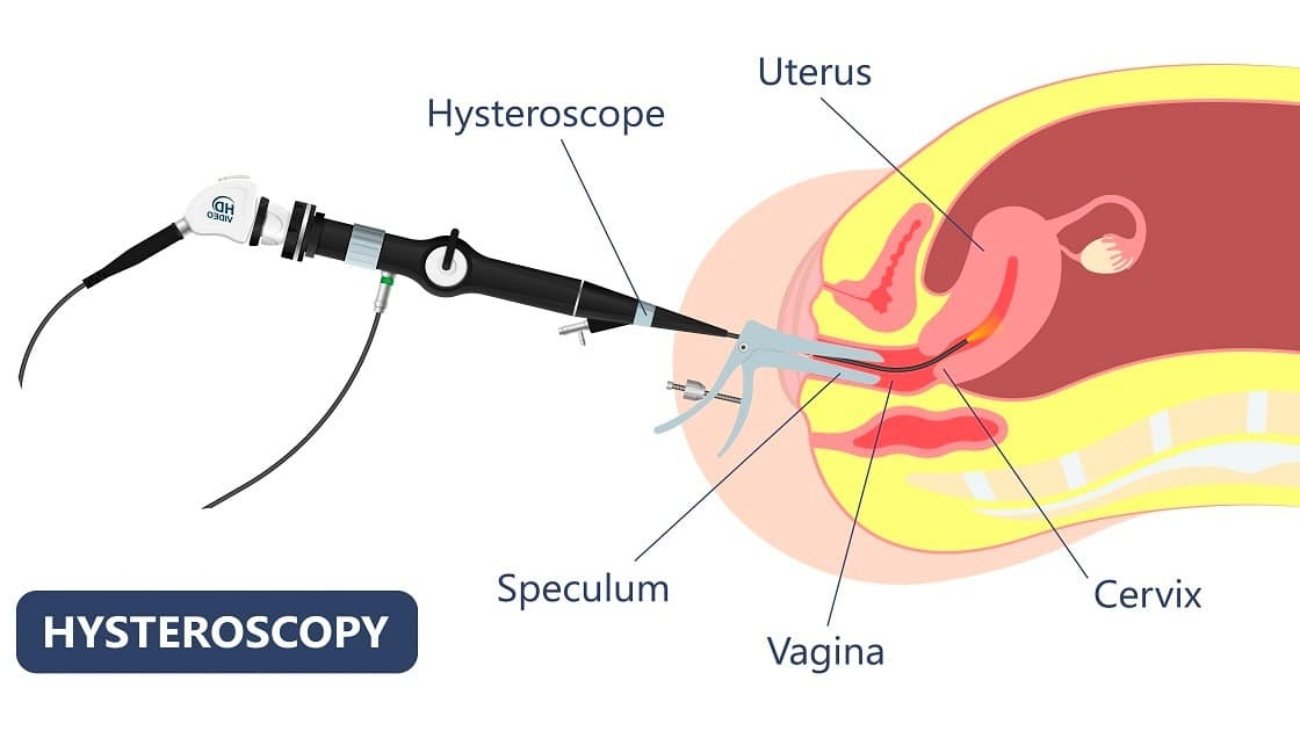
Ultrasound
Used to identify structural issues like varicocele.
Treatment Options for Low Sperm Count
Treatment depends on the underlying cause.
Lifestyle Changes
- healthier diet
- exercise
- weight management
- stress reduction
- sleep improvement
Medical Treatment
Doctors may recommend:
- hormonal treatment
- supplements
- infection treatment
- fertility medications
Advanced Fertility Treatment
Some couples may require:
- IUI
- IVF
- ICSI
depending on sperm quality and fertility goals.
Learn more about fertility treatment →
Kore Fertility Solutions
Foods That May Support Sperm Health
A fertility-friendly diet may include:
- fruits and vegetables
- nuts and seeds
- protein-rich foods
- zinc-rich foods
- antioxidants
- hydration
Lifestyle improvement plays a major role in long-term reproductive health.
Male Fertility Myths Men Should Stop Believing
“Infertility Is Always a Woman’s Problem”
False. Male factors contribute to many infertility cases.
“Healthy Appearance Means Healthy Fertility”
False. Fertility problems can exist without visible symptoms.
“Low Sperm Count Means No Pregnancy”
False. Many couples conceive successfully with proper treatment.
When Should You See a Fertility Specialist?
Consult a fertility expert if:
- pregnancy is not happening after 1 year
- there is erectile dysfunction
- ejaculation problems occur
- testicular pain persists
- previous fertility issues exist
Early diagnosis improves treatment outcomes significantly.
Not Sure About Your Fertility Health?
Don’t ignore the signs. Fertility evaluation can help identify underlying issues early.
Talk to a Fertility Specialist →
Book Consultation
Call Now: +91 98889 91413
Why Couples Trust Dr. Nitasha Gupta
Patients across Panchkula, Chandigarh, Mohali, Zirakpur, and Tricity trust Kore Fertility Solutions for advanced fertility evaluation and personalized reproductive care.
Treatment plans focus on:
- evidence-based fertility care
- advanced reproductive technology
- ethical guidance
- couple-focused treatment planning
Read reviews & clinic directions →
Google Reviews – Dr. Nitasha Gupta
FAQs
Can low sperm count be improved naturally?
Yes. Lifestyle changes, diet improvement, exercise, stress reduction, and medical treatment may improve sperm health.
Does stress affect sperm count?
Yes. Chronic stress may affect hormones and fertility health.
Can low sperm count still lead to pregnancy?
Yes. Many couples achieve pregnancy naturally or with fertility support.
Which test checks male fertility?
Semen analysis is the most common fertility evaluation test for men.
Is low sperm count common?
Yes. Male fertility problems are increasingly common due to lifestyle, stress, and health factors.
Medical Disclaimer
This content is intended for educational purposes only and should not replace professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare professional for personalized guidance.