Is Laser Vaginal Tightening Safe? – Medical Safety Guide (2026)
Laser vaginal tightening has emerged as one of the most searched procedures in cosmetic gynecology — particularly among women seeking non-surgical solutions for vaginal laxity, dryness, and intimate wellness.
However, the most critical clinical question remains:
Is laser vaginal tightening actually safe?
Short Answer – Medical Safety Verdict
Yes — laser vaginal tightening is considered safe when performed by certified gynecologists using FDA-approved medical laser technology under sterile clinical protocols.
Safety risk increases significantly when procedures are conducted:
- In cosmetic spas
- By non-medical staff
- Using uncertified devices
Medical supervision is the primary determinant of procedural safety.
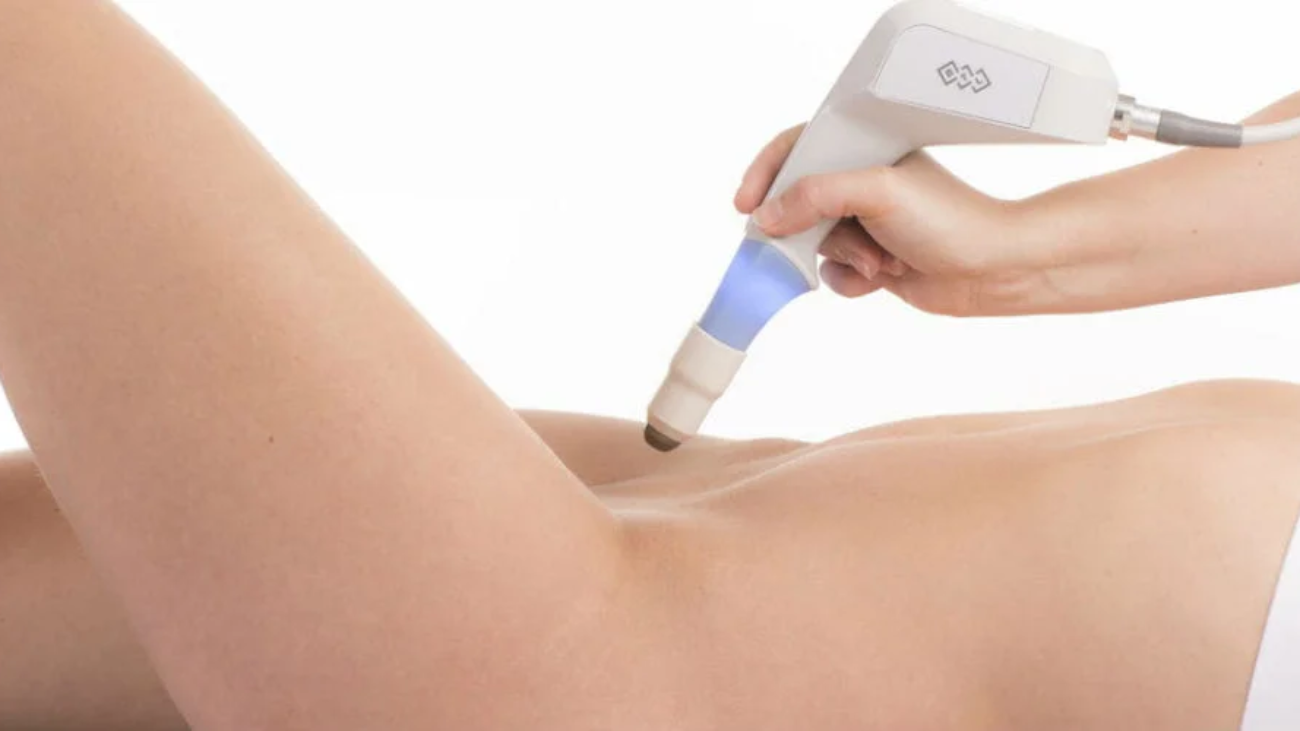
What Is Laser Vaginal Tightening?
Laser vaginal tightening is a non-surgical treatment that uses controlled fractional laser energy to stimulate collagen remodeling within vaginal mucosal tissue.
This leads to:
- Improved elasticity
- Tissue tightening
- Increased lubrication
- Enhanced vascular circulation
The procedure is commonly chosen for women experiencing:
- Post-childbirth vaginal looseness
- Age-related laxity
- Vaginal dryness
- Mild urinary leakage
- Reduced intimate comfort
What Makes Laser Vaginal Tightening Safe?
Safety is protocol-dependent — not procedure-dependent.
H3 – 1. Gynecologist Supervision
Only trained gynecologists possess expertise in:
- Vaginal anatomy
- Nerve mapping
- Tissue response thresholds
Procedures performed without medical oversight carry higher complication risk.
2. FDA-Approved Technology
Certified clinics use regulated energy-based devices that control:
- Thermal depth
- Pulse duration
- Tissue exposure
External reference on device safety standards:
American College of Obstetricians & Gynecologists (ACOG)
https://www.acog.org
FDA device clearance database:
https://www.fda.gov/medical-devices
3. Patient Screening
Pre-procedure evaluation ensures exclusion of:
- Pregnancy
- Active infections
- Cervical pathology
- Uncontrolled diabetes
Screening minimizes adverse outcomes.
4. Clinical Energy Dosing Protocol
Laser settings must be individualized based on:
- Tissue laxity grade
- Hormonal status
- Age
- Obstetric history
Standardized “one-setting-fits-all” treatments are unsafe.
Is the Treatment Painful?
No.
Most women report:
- Mild warmth sensation
- No pain
- No anesthesia requirement
- No injections
The procedure is OPD-based and lasts ~20–30 minutes.
Common Side Effects
When performed under medical protocols, side effects are mild and temporary:
- Warmth for a few hours
- Mild swelling
- Watery discharge (24 hrs)
- Temporary sensitivity
Serious complications are extremely rare in gynecologist-led settings (confidence interval: <1–2% minor adverse events in device trials).
How Many Sessions Are Needed?
Standard therapeutic protocol:
- 2–3 sessions
- Spaced 4–6 weeks apart
Collagen regeneration continues for weeks post-procedure.
Who Should Avoid Laser Vaginal Tightening?
Treatment may be deferred in:
- Pregnant women
- Active vaginal infections
- Untreated cervical disease
- Recent pelvic surgery
- Uncontrolled chronic illness
Eligibility is determined after gynecological evaluation.
Is Laser Vaginal Tightening Effective?
Clinical and patient-reported outcomes show improvement in:
- Vaginal tone
- Elasticity
- Lubrication
- Mild stress urinary leakage
- Intimate comfort
Urogynecological literature demonstrates progressive collagen remodeling over 8–12 weeks post-therapy (moderate evidence strength).
External clinical reference:
International Urogynecological Association (IUGA)
https://www.iuga.org
Safe Laser Treatments in Dhakoli – Specialist Care
Laser vaginal rejuvenation performed at
LaBella – Cosmetic Gynecology & Intimate Wellness
is conducted strictly under certified gynecological supervision.
Associated fertility and women’s health care support is available via
Kore Fertility Solutions Pvt. Ltd
Under the expertise of
Dr. Nitasha Gupta
Gynecologist & Intimate Wellness Specialist serving Dhakoli, Zirakpur, Panchkula, Chandigarh & Mohali.
Recovery & Downtime
- Resume routine activities same day
- Avoid intercourse: 3–5 days
- Avoid tampons/sauna: short term
No hospitalization required.
FAQs – Laser Vaginal Tightening Safety
Is laser vaginal tightening FDA approved?
Yes — several laser platforms used for vaginal rejuvenation are FDA-cleared for gynecological use when applied under medical supervision.
FDA device database:
https://www.fda.gov/medical-devices
Is downtime required?
No downtime. Patients resume daily routine immediately with minor precautions.
Is there permanent damage risk?
Permanent injury is extremely rare when procedures are performed:
- By certified gynecologists
- Using approved devices
- Under sterile clinical protocols
Book Professional Consultation
For confidential laser vaginal rejuvenation under certified supervision, consult:
LaBella – Cosmetic Gynecology & Intimate Wellness
099883 09211
Private • Ethical • Gynecologist-Led